Open Minds
Mental health and wellbeing in policy and practice

CONTENT WARNING
Please be aware that this collection includes articles on topics that may cause distress, including mental illness, suicide, and self-harm.
Contents
Foreword
Mark Rowland, CEO, Mental Health Foundation
LGBT+ inequalities in adolescent wellbeing
Professor Neil Humphrey
Psychedelics for mental health
Tripping over red tape
Professor Jo Neill
Fighting the war with drugs
How can psychedelic-assisted therapies help veterans?
Professor Jo Neill, Dr Verity Wainwright, Frances Smith
Suicide prevention for veterans of the UK Armed Forces
Adding to the national evidence base
Dr Cathryn Rodway and Dr Jodie Westhead
What we need to know next about loneliness
Professor Pamela Qualter
Why do teachers need to think about student experiences of loneliness?
Professor Pamela Qualter, Dr Rebecca Jefferson, and Dr Lily Verity
All sorted now?
The continued risk of COVID-19 to patients with severe mental illness
Dr Lamiece Hassan and Dr Joseph Firth
Mind your language
Interpreters in Mental Health Act assessments
Professor Alys Young, Dr Rebecca Tipton, and Dr Natalia Rodríguez-Vicente
Locked up like adults
COVID-19 experiences for children in custodial settings
Dr Charlotte Lennox
Mind the gap
Supporting prison leavers with mental illness
Dr Jane Senior, Professor Jennifer Shaw, and Dr Charlotte Lennox
Foreword
Mark Rowland, CEO, Mental Health Foundation
We have made huge progress in improving physical health in this century and the last one. Blights such as child mortality and deaths from infectious diseases have declined sharply in most parts of the world. But mental health is going in the wrong direction.
When I started to work in mental health in 2016, the World Health Organization predicted that depression would be the leading cause of ill-health by 2030. We have already reached that mark. In England, around 1.2 million people are currently on NHS waiting lists, and millions more are struggling with diagnosable levels of mental ill-health but getting no support at all. Of particular concern is the rising prevalence of mental health problems among young people. In 2017, the NHS estimated that approximately 10% of 17- to 19-year-olds had a mental disorder. By 2022, following the pandemic, this figure had risen to a troubling 26%.
It’s not just prevalence that’s on the rise: severity is increasing as well. Hospital admissions for eating disorders surged by 84% over the period 2015/16 – 2020/21, reaching 24,268 admissions. Again, children and young people were the worst affected with a rise of 90% in the five-year period.
Mental health problems do not only create suffering in the mind; they can also worsen physical health conditions. And Mental Health Foundation research found that they carry a social and economic cost of £118 billion every year.
But as a country, we are looking through the wrong end of the telescope. We consistently fail to invest in health creation and prevention and then pick up the cost. We allocate approximately £230 billion to healthcare but only about £3.5 billion to public health, with a mere 2% of that dedicated to public mental health initiatives.
The evidence base for preventing mental health problems is steadily growing. There are a good number of interventions like workplace support initiatives, anti-bullying programmes, and better perinatal mental health support, where the evidence is very clear. Governments and health systems should urgently invest in these solutions. And we know that the toxic impacts of poverty and discrimination are two of the most important drivers of mental ill-health; any cross-government plan must ensure that these are priorities.
But we need to keep pushing the evidence further, harness new technologies and re-engineer our health systems to prioritise tackling the rising number of mental health problems in our society. We need new tools and new thinking. And we need to leave no inequality unaddressed in both the prevention and treatment of mental health problems.
That’s why the work of Policy@Manchester is so vital. There are some brilliant ideas in this report. Some of them are common-sense, like supporting our veterans better and reducing loneliness. Some will be unconventional, like exploring the use of psychedelics in treatment. But we need to follow the evidence, rigorously interrogating ideas and adopting them where they can be shown to be useful. In keeping with the title of this collection: let’s keep open minds.
LGBT+ inequalities in adolescent wellbeing
Professor Neil Humphrey
Improving wellbeing in every area of the UK is the overarching ambition of the Levelling Up White Paper, and government has said it will undertake further work to supplement existing wellbeing data at a subnational level. In Greater Manchester, a community-led, hyper-local project is underway to understand and improve children and young people’s wellbeing, and some of the approaches and early data can provide ideas for levelling up mental health. In this article, Professor Neil Humphrey, academic lead for #BeeWell, reflects on a recent analysis of wellbeing inequalities for young people across Greater Manchester, focusing in particular on disparities experienced by LGBT+ young people, and considers how they should be addressed.
- In autumn 2021, we surveyed nearly 40,000 young people from more than 160 secondary schools across all ten local authorities (LAs) in GM to ask about their wellbeing.
- Only 7% of boys report a high level of emotional difficulties, compared with 22% of girls and 50% of non-binary young people.
- Gay, lesbian, bi and pansexual young people scored, on average, less than 5 out of 10 on our life satisfaction measure, compared to around 7 out of 10 for their heterosexual peers.
- In order to address these inequalities, we must work with young people to identify solutions and take a whole community approach, involving local and regional authorities, charities, researchers and schools, to support their wellbeing.
What is #BeeWell?
#BeeWell is a programme that aims to make the wellbeing of young people everybody’s business. We are assessing their wellbeing on an annual basis via a co-produced survey and aim to use the data generated to bring about positive change in Greater Manchester’s (GM) schools and communities as a result.
In autumn 2021, we surveyed nearly 40,000 young people from more than 160 secondary schools across all ten local authorities (LAs) in GM. Data results were analysed using robust statistical methods that quantified wellbeing inequalities across gender identity, sexual orientation, ethnicity, language, age, socio-economic status, caregiving responsibilities, and special educational needs and disabilities (SEND). For this analysis, we focused on the following domains:
- Life satisfaction – quality of life as a whole
- Psychological wellbeing – feeling good and functioning well
- Stress – feeling overwhelmed by the demands of daily life
- Negative affect – experience of difficult emotions such as sadness and worry
What did we find?
In our recent evidence briefing, we identified major wellbeing inequalities in relation to gender identity and sexual orientation.
There are gaps in wellbeing scores between males and females. For example, girls’ average life satisfaction score was 6.2 out of 10, whereas boys scored 7.2. Only 7% of boys reported a high level of emotional difficulties compared with 22% of girls. Non-binary young people also report lower levels of wellbeing than boys, with even more pronounced differences. For example, 50% of non-binary young people reported a high level of emotional difficulties, and they score, on average, more than 3 points lower on our psychological wellbeing measure. Meanwhile, transgender young people reported significantly higher stress levels than those who are cisgender.
There are also sizeable wellbeing inequalities for young people when focusing on sexual orientation. For example, gay, lesbian, bi and pansexual young people scored, on average, less than 5 out of 10 on our life satisfaction measure, compared to around 7 out of 10 for their heterosexual peers.
Finally, our analyses identified wellbeing inequalities across ethnicity, SEND, caregiving responsibilities, socio-economic status, and age. However, these were much smaller in magnitude than disparities relating to gender identity and sexual orientation.
Why do these wellbeing inequalities exist?
#BeeWell survey data shows differences in wellbeing but not the reasons behind them. So we are working with a coalition of partners and young people in GM to explore how to address the findings.
Lisa Harvey-Nebil, Chief Executive Officer from The Proud Trust has noted: “As an LGBT+ youth charity we were not surprised that LGBT+ young people report feeling less satisfied with their lives than their counterparts. These results align with our own research findings conducted with young people attending our provision during the pandemic. Our research highlighted that 21% of LGBT+ young people had experienced more LGBT-phobia during the pandemic, with 76% saying their mental health had worsened during that time.”
Simone, a Proud Trust young person, reflects: “education establishments need to look at themselves, their spaces, the culture they foster, and the training they provide their staff to ensure that it is LGBT+ inclusive, making it a happier and safer environment for LGBT+ young people”. Outside of education, Simone says, “Material change for transgender lives would show young trans and non-binary people that their needs are being met, that their problems are considered to have equal weight to their cisgendered counterparts.”
How can we support the wellbeing of LGBT+ young people?
Now that we have initial findings from the survey, #BeeWell partners are in early stages of using those findings to support young people’s wellbeing. Some of the approaches we are taking can act as a model for similar initiatives across the country and there are also broader areas for consideration.
Young people must be involved in creating solutions. The voice of young people is critical to the success of any wellbeing programme. An example of how we have done this with #BeeWell is to have young people sitting on our governance boards, holding the programme accountable to its aims and co-creating our survey. Any programme of work to support young people must include young people. For example, in response to our findings, the Greater Manchester Health and Social Care Partnership have created a youth-led commissioning pot for activities to support LGBT+ young people’s wellbeing.
A whole community approach is necessary to truly support our young people. The #BeeWell project team consists of a team of experts in wellbeing and education across local government, the University and charities. By working with schools, local authorities, and other organisations in Greater Manchester, we can use this data to direct services in the right places and help schools to identify and support their students. Addressing LGBT+ inequalities in wellbeing is an example of how we are taking this approach. By working with organisations such as The Proud Trust, who are experts in the inequalities our data has highlighted, we can combine our knowledge to provide support for young LGBT+ people. This is something that couldn’t be done without collaboration with people with lived experience and organisations that work with communities whose wellbeing is impacted.
Collecting new data as well as analysing existing data. Linking in with the Levelling Up White Paper, the ONS has created the Subnational Indicators Explorer, which breaks down data to regional and local authority (LA) level. While it wouldn’t be feasible for the ONS to break down data to an even more local level, it could provide information on how and where combined authorities, LAs, researchers, schools and voluntary and community organisations can access data that is either gathered or disaggregated at a local level. Data collected in a place, co-designed by the people living there, can add extra layers of information and nuance.
Prioritise addressing gender and sexual orientation wellbeing inequalities in the mental health component of the Major Conditions Strategy (MCS). Both the call for evidence and discussion paper for the 10-year Mental Health Plan which fed into the MCS reference gender and sexual orientation disparities, among others like socio-economic disadvantage and ethnicity. However, our findings indicate gender identity and sexual orientation should be given more prominence as part of a wide-ranging strategy to promote positive mental wellbeing and prevent mental ill-health. Key to any strategy will be intervening to address the factors that underpin the wellbeing inequalities LGBT+ young people experience, such as higher levels of bullying and discrimination.
Evaluate the impact of the Relationships and Sex Education (RSE) statuary guidance. The RSE guidance should be helping to improve pupils’ wellbeing and should make schools more LGBT+ inclusive, but the initial findings from our survey suggest this may not be the case. The Department for Education should evaluate the impact of guidance so far and on a long-term basis to see how it is affecting young people’s wellbeing, understanding and experiences, and amend guidance if it finds that not all students have the opportunity to learn about LGBT+ relationships.
This article is based on the first year of data for the #BeeWell programme. Data from the 2022 survey confirmed these findings, and provided further insight into the role of neighbourhoods in young people's wellbeing. You can read more about this in our publication, Power in Place.


Psychedelics for mental health
Tripping over red tape
Professor Jo Neill
The last decade has seen a new focus on psychedelics as powerful medicines for treating severe mental health issues, including the use of psilocybin for conditions such as PTSD and treatment-resistant depression. However, many of these potentially life-saving treatments, including psilocybin, remain difficult to research due to overly strict drug laws. In this article, Professor Jo Neill outlines the evidence-based case for the rescheduling of psilocybin and other drugs, including the benefits they can bring to health, national prestige, and the UK economy.
- Poor mental health currently costs the UK economy upwards of £100 billion per year due to losses in productivity.
- Psilocybin-assisted therapy for depression has shown more than 70% long-term efficacy.
- Despite the huge potential of psilocybin and other psychedelics, current drug control laws in the UK are unnecessarily restricting research into this area.
- Reforming the UK’s drug scheduling laws would bring the country in line with the US, Germany, and others, with benefits to health, British research, and the economy.
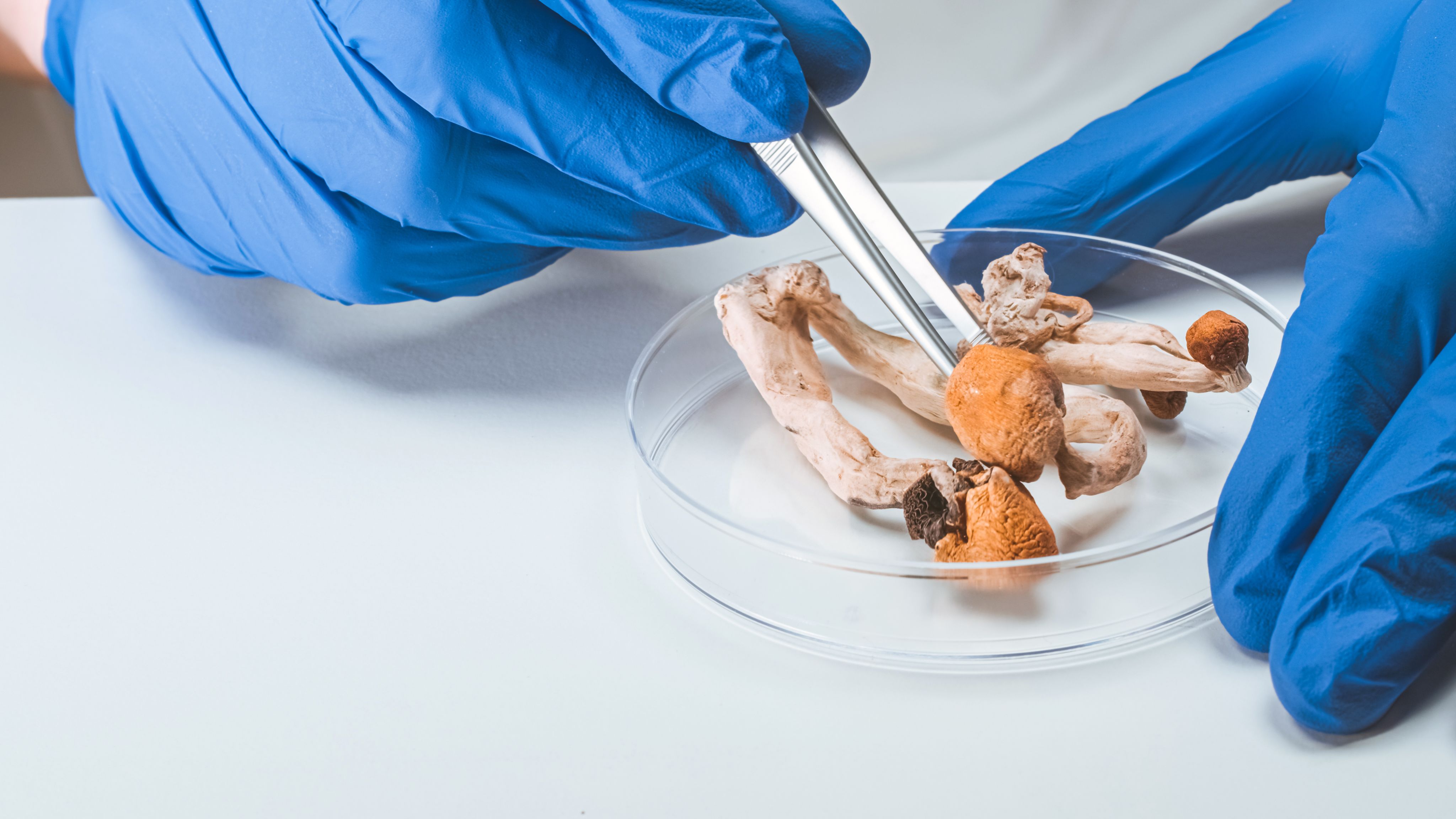
Medical psychedelic research has undergone a renaissance in recent years. Psychedelics include plant medicines such as psilocybin (the active constituent of magic mushrooms), Ayahuasca (a powerful psychedelic used by indigenous populations, often consumed as a tea), and those synthesised in the laboratory, including LSD and MDMA (ecstasy). Psilocybin is a naturally occurring molecule found in over 200 species of fungi. It is structurally similar to serotonin – a human neurotransmitter that regulates mood and perception. When administered in clinical settings with psychological support, early clinical trials show that psilocybin may be a safe and effective treatment for many mental health disorders, particularly for patients for whom other treatments have been ineffective.
Psilocybin for mental health
These medicines are, in recent small scale clinical studies, proving to be very effective for hard-to-treat psychiatric conditions, such as severe depression, anxiety and depression that occurs in terminal cancer patients, alcohol and nicotine dependence, and OCD (obsessive compulsive disorder). Most recently, evidence is emerging for efficacy in PTSD (post-traumatic stress disorder).
Our focus is on psilocybin, as the psychedelic drug with most clinical evidence for its effectiveness for severe depression. Unfortunately, researching psychedelics is particularly difficult in both human and animal studies. It is extremely costly, bureaucratic, and incurs large time delays due to its current status as a Schedule 1 drug under the Misuse of Drugs Regulations of 2001. This stems from its classification as a Class A drug under the Misuse of Drugs Act 1971, in turn based on the UN drug control conventions of 1960 and 1971. These conventions detail the scheduling of different controlled drugs at the international level. Drugs are divided into five schedules, each specifying how national governments should regulate such activities as import, export, production, supply, possession, and record keeping which apply to them, for example in research-based circumstances. At both the UK and UN level, psilocybin is currently in Schedule 1, which has the most stringent regulations, while some drugs that are in Schedule 2 – and therefore have more relaxed requirements – are heroin, fentanyl, cocaine, and ketamine.
Given the significant clinical evidence for its efficacy as a treatment for mental health conditions, we are calling for the laws in the UK to be changed to enable research with psilocybin.
Drug scheduling
For substances in Schedule 1, a Home Office licence is generally required for their production, possession, or supply. A controlled drug register must be used to record details of any Schedule 1 controlled drugs received or supplied by a pharmacy. Researchers seeking to work on potential new treatments for treatment-resistant depression (TRD) using psilocybin face burdensome additional costs and delays, stemming from its classification as a Schedule 1 substance. This is in spite of existing evidence of medical benefit and its potential as the basis for new treatments for this illness. Demonstrating this is not a theoretical issue – it already determines which research projects researchers choose to consider, which get approved, and how billions of pounds of R&D funds in the UK and international pharma industry are committed.
In order to enable this research in the UK, this Government needs to remove psilocybin from Schedule 1 of the Misuse of Drugs Regulations 2001.
Science has moved on, there is now sufficient evidence of potential medical benefit for medicines derived from psychedelics. Moving psychedelics from Schedule 1 to a lower Schedule would enable our drug regulations to continue working in the way that they were intended – allowing medical and pharmaceutical research, and continuing to guarantee secure and responsible stewardship of substances in a small number of properly regulated organisations.
By rescheduling psilocybin to Schedule 2, many opportunities can be realised. There will be benefits not just in the field of health and social care, but also economic, industrial, and financial rewards.
Benefits of rescheduling
The most obvious benefit of rescheduling will mean that research can more easily be conducted into the effectiveness of psilocybin for mental health treatments. Mental health has reached crisis levels during the COVID-19 pandemic. 21% of adults experienced depression during 27 January to 7 March 2021; an increase of 11% from pre-COVID levels (10%). Psilocybin-assisted therapy is one of the most promising innovations for the treatment of depression seen for decades, with greater than 70% long-term efficacy in small scale trials to date. These long-term effects could result in a reduction in future spending on mental health treatments, and can also contribute to workforce health and productivity. Poor mental health currently costs the UK economy upwards of £100 billion per year due to losses in productivity. By using psilocybin as a long-term strategy, it has the potential to solve these interlinked problems in one go. Research from the United States has shown that psilocybin-assisted therapies may also be used safely and be effective for substance-misuse disorders, end-of-life anxiety and obsessive-compulsive disorder.
While it could contribute to a general increase in mental health outcomes, it could also have enormous benefits for service veterans. Currently, some veterans who return from their active duty suffer from mental illnesses, most commonly PTSD. The treatments that the UK has to offer frequently aren’t effective enough, so these veterans seek help elsewhere. Many UK veterans make use of psilocybin retreats in the Netherlands – where psilocybin is legal – to self-treat their own mental health illnesses. It is not right that UK veterans who risked their lives are having to leave the country to access this treatment.
Although there are obvious benefits for mental health, rescheduling psilocybin makes economic sense too. The Government has identified Life Sciences and pharmacy as a flagship UK industry in the post-Brexit period, which rescheduling psilocybin could be a large part of. For years now, the UK has been falling behind many other countries on research and development spending. The window is closing to be an international leader, with competition from the US, Germany, and others, as there will be a ‘first in market’ advantage for whoever acts decisively to enable this research at scale. In doing so, the potential for new research jobs, both in higher education and in industry, is created, contributing further to the UK’s productivity. Changing this law has never been more pertinent.
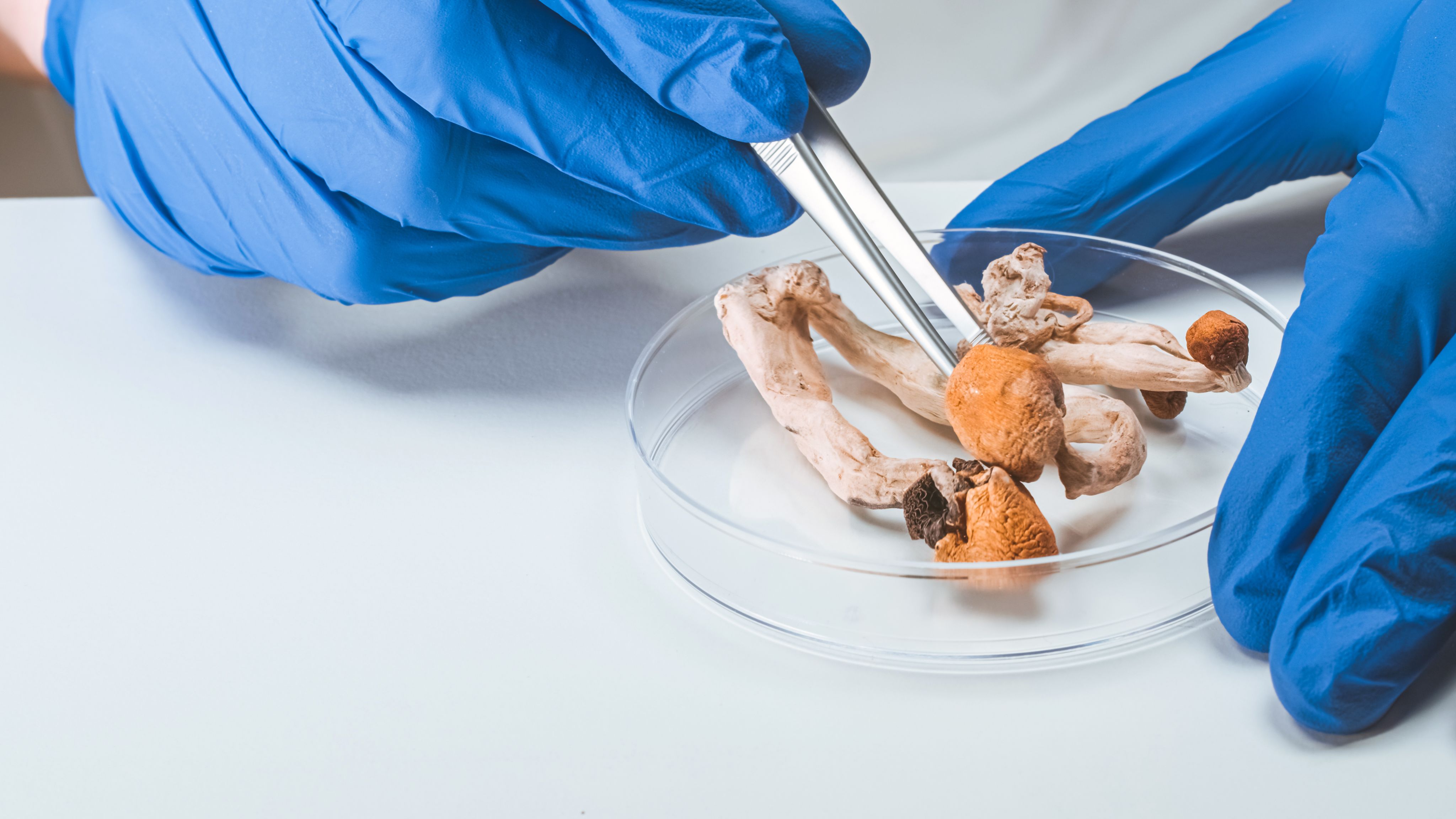

Fighting the war with drugs
How can psychedelic-assisted therapies help veterans?
Professor Jo Neill, Dr Verity Wainwright and Frances Smith
Around 17% of recent military veterans in the UK report symptoms of post-traumatic stress disorder (PTSD) and currently available treatments don’t work for many of these. Here, Professor Jo Neill, Dr Verity Wainwright, and Frances Smith report the findings of a new study into the role that psilocybin (the active constituent of so-called ‘magic’ mushrooms) can have in the treatment of PTSD symptoms in veterans, and how the law can be updated to enable more research in this area.
- Psychedelic-assisted psychotherapy for PTSD shows potential as an effective, long-term treatment.
- Crucially, it offers an acceptable alternative to current treatment options for military veterans.
- But bureaucratic barriers are slowing research into this area in the UK.
When transitioning back into civilian life, some military veterans experience issues with their mental health, including symptoms of trauma. While many former service personnel with PTSD benefit from the treatment options currently available to them, a number report finding these options difficult to access, not effective, or not acceptable to them. Alternative forms of treatment are needed for those not benefitting from, or engaging with, current options.
There is emerging evidence for the efficacy of psychedelic medicines – in combination with clinical psychotherapy – for the treatment of a range of mental health conditions, including PTSD.
“There’s just no such thing for me as PTSD anymore”
Researchers from The University of Manchester interviewed seven ex-armed forces personnel with either current or previous symptoms of trauma. Five of them had previously used psilocybin to self-medicate, while two had considered doing so. All of them said they had struggled to access treatment on the NHS, or had found previous attempts at treatment unsuccessful.
“I didn’t want to go onto antidepressants, because I’ve had a lot of friends who have been on antidepressants and all of the other pills they give you and all I’ve seen is them mess them up worse than when they started them.”
– ‘Tom’
Several said they had turned to psilocybin in desperation. Of those who had used psilocybin, all of them said they had experienced both immediate and long-lasting positive effects on their mental health and trauma symptoms.
“There’s just no such thing for me as PTSD anymore … if you use psychedelics, you can walk all over it, look at it at the floor around you and then just choose to scoop up all those piles of trauma and stuff, put it in a folder and it’s up to you, you can carry that around with you or not.” – ‘Nick’
The mechanism by which psilocybin acts on the brain is still being studied, but the effect is to increase neuroplasticity – the brain’s ability to reform and make new connections. This increased neuroplasticity is associated with patients’ ability to break out of harmful thought patterns following psychedelic-assisted psychotherapy (PAP), and may also explain why relapse rates following PAP are significantly lower than for other treatments.
This long-term efficacy is another reason for the attractiveness of psychedelic treatments for veterans. As ‘Chris’ put it;
“… not very many people who I am aware of in the military are very interested in taking antidepressants long-term, there’s a lot of shame associated with that… it’s appealing that psilocybin could be a treatment that would work with a with a singular, you know, it happens once and then you’re just, that’s it, you’re treated … that appeals to me and I think that that would appeal to service personnel and make them a lot more likely to seek help.”
Anecdotally, a growing number of veterans are now turning to psychedelics to self-medicate, either by purchasing them illegally in the UK, or travelling to countries where psychedelics have been decriminalised, such as the Netherlands. Some charities have begun providing support for veterans and emergency workers seeking to access psychedelic-assisted psychotherapy, including psilocybin retreats in the Netherlands, as well as ayahuasca (an indigenous South American psychedelic substance).
Veterans are not the only group who may benefit from new treatments for trauma-related conditions – between 22% and 44% of frontline care staff in the NHS reported symptoms consistent with PTSD as a result of their experiences during the COVID-19 pandemic.
Change begins in the Home (Office)
Despite growing evidence for the medicinal potential of psilocybin and other psychedelic substances, the UK has maintained their status as a Schedule 1 controlled substance. This category is reserved for drugs with “no medical value” – something psilocybin clearly has. While it is possible to conduct research with Schedule 1 drugs, the financial and bureaucratic hurdles to be overcome are a major barrier to smaller Universities and pharmaceutical companies. Meanwhile, heroin, cocaine, and ketamine are all under Schedule 2, and are therefore subject to less restrictions despite being consistently demonstrated as more harmful substances.
In response to a recent petition on rescheduling of psilocybin, the Home Office stated that it will review the Schedule 1 status of psilocybin as and when a medicine is approved for market by the Medicines and Health Products Regulatory Agency (MHRA). However, it is the Schedule 1 status – and the barriers this creates to scientific and medical research – that is slowing the development of psychedelic-derived medicines to be presented to the MHRA.
Internationally, there is growing evidence that psychedelics – taken in controlled settings alongside therapy – represent a paradigm shift in the way mental health conditions are treated. The UK has the life sciences infrastructure and expertise to be a global leader in this new environment, but is held back by unnecessary red tape that is not supported by the scientific evidence.
To remove these barriers, the Home Office should grant an exemption to psilocybin’s Schedule 1 status for the purpose of medical and scientific research. Universities already have an exemption for research involving Schedule 2 drugs, and have proved that they can handle illegal compounds safely and sensibly.
In three years or thirty?
The UK has both the potential and the need to be at the forefront of this. COVID-19 has escalated an already substantial mental health burden, with veterans only one of many groups affected by trauma, anxiety, and depression. Not only could a scheduling exemption increase the UK’s global research prestige, but it could also ensure new treatments are available on the NHS, so those who need them can access them.
With companies and institutions around the world investing in psychedelic medicines, it is inevitable that a treatment will eventually make it to market and fulfil the requirements set by the Home Office on the MHRA. The question is whether this takes years or decades, and if the UK will fulfil its potential as a global pioneer of good mental health. The answer lies with the policymakers.


Suicide prevention for veterans of the UK Armed Forces
Adding to the national evidence base
Dr Cathryn Rodway and Dr Jodie Westhead
There are no recent UK-wide studies, and comparatively few international ones, examining suicide in military veterans. This is despite increasing public concern about suicide and the mental health impact of serving in the UK Armed Forces, particularly following a period of intensive operations in Iraq and Afghanistan. The recently published National Suicide Prevention Strategy for England sets out an ambition to better understand suicide rates in veterans within the next 5 years, while the 2022-2024 Veterans Strategy Action Plan outlines the steps needed to transform services and support for veterans by 2028. In this article, Drs Cathryn Rodway and Jodie Westhead, researchers at the National Confidential Inquiry into Suicide and Safety in Mental Health (NCISH), explain how their work adds to the evidence base of suicide prevention in veterans of the UKAF.
- Researchers from The University of Manchester examined the risk of suicide in veterans compared to the general population, and investigated factors most associated with suicide after discharge.
- The overall risk of suicide in veterans is not higher than the generation population, but young men and women leaving the Armed Forces are at higher risk, especially if they had short lengths of service.
- Improving and maintaining access to mental health care and social support for young service leavers, combined with implementing general suicide prevention measures for all veterans regardless of age, is important for suicide prevention in this group.
What was the purpose of the research and why is it important?
There is a lack of global consensus on whether past military service increases suicide risk. Research suggests veterans of the Armed Forces may be a potentially vulnerable group for many reasons, including traumatic life events prior to enlisting, unique experiences while in Service, the difficulties associated with returning to civilian life and high rates of unemployment, homelessness, and alcohol and drug misuse following discharge. In a previous 10-year study (1996-2005) of almost 234,000 people who left the Armed Forces, 0.1% died by suicide, and the overall suicide rate was no greater than in the general population.
Over 15 years have passed since then, and the military context in the UK has changed, as have patterns of suicide in the general population. There has been concern about the mental health impact of serving in conflicts in Iraq and Afghanistan, the number of full-time personnel in the Army has decreased, and there are more specialist NHS health and other third-sector support services available for veterans. It was in this new context that we undertook our latest research.
Suicide in veterans – rates and risk factors
In our recent study we looked at data for over 458,000 veterans who left the Armed Force between 1996 and 2018 (an additional 13 years of data compared to our previous study, and over 200,000 more veterans). In this 23-year period, 1,086 (0.2%) veterans tragically took their own lives. We found the overall rate of suicide in veterans was slightly lower than the general population, but identified differences according to age. Suicide risk was 2-3 times higher in male and female veterans aged under 25 compared to the same age-groups in the general population. Male veterans aged over 35 were at reduced risk of suicide.
We identified some factors which increased suicide risk in veterans, including being male, serving in the Army, having served for less than 10 years, being discharged from the military before the age of 35 years, and being untrained. However, there were also some factors which appeared protective – being married, of a higher rank, and serving in a conflict appeared to reduce suicide risk.
A quarter (273/1,086; 25%) of veterans who died by suicide had been in contact with specialist NHS mental health services in the 12 months before death (i.e., were patients), similar to the general population (27%). Of note, however, was our finding that the rate of contact with these services was lowest (21%) in the age-group most at risk (veterans aged under 25), suggesting younger veterans in particular may not be seeking help. Compared to non-veterans who died by suicide within 12 months of contact with mental health services, veterans of the Armed Forces more often had a diagnosis of depression or bipolar disorder (33% vs 27%) and evidence of PTSD, although numbers were small (3% vs 1%). There were few other differences and levels of unemployment, alcohol and drug misuse, and self-harm were similar to patients who had not served in the Armed Forces.
What does this mean for prevention?
Our research suggests the highest risk of suicide continues to be in young veterans, and young people who serve for short lengths of time may have the most pressing needs. However, 16–24-year-olds made up 18% of the total veteran population who died by suicide, compared to 26% of 40–54-year-olds (although rates were lower in the older age group), suggesting all veterans regardless of age should be the focus of prevention. The low rate of contact with specialist NHS mental health services suggests veterans may not be seeking help, or may not be aware of the help that is available.
Improving access to (and knowledge about) mental health care, and encouraging help-seeking or campaigns to reduce stigma may increase engagement in veterans. However, equipping services with the knowledge and training to better support the health of veterans and understand their culture and needs is also important, as is services having the information to signpost veterans to financial advice, housing and employment support. Implementing general suicide prevention measures like tackling self-harm, alcohol and drug misuse and enhancing social support, is as important for veterans as it is for the general population.
Delivering on these recommendations will require cross-departmental working between the Ministry of Defence (particularly the Office for Veterans Affairs), the Department of Health and Social Care, and local & national health and care services (such as the 42 Integrated Care Services in England, and OpCOURAGE, the dedicated NHS service for the Armed Forces). A clear process, developed and agreed by these stakeholders, should be in place to provide services and advice to veterans upon leaving the Armed Forces.
Our recent study is one part of understanding the causes of suicide in veterans of the Armed Forces. Further research by The University of Manchester will explore the role of pre-service or other factors that may have influenced later suicide risk, such as childhood trauma or homelessness. New methods of recording veteran suicide, announced in 2021, will also better our and service providers understanding of the needs of veterans.


What we need to know next about loneliness
Professor Pamela Qualter
The COVID-19 pandemic has had a profound impact on the UK’s mental health, particularly loneliness. Data from spring 2021 found a million more adults were feeling lonely “often” or “always” compared to spring 2020. Now, a recent evidence review for DCMS, led by Professor Pamela Qualter, has set out what we know – and don’t know – about loneliness in the UK, and suggests priorities for policymakers in tackling this vast problem.
- Loneliness costs the UK up to £2.5 billion each year, through lost productivity, staff turnover, and other effects.
- Loneliness has increased during the COVID-19 pandemic, with between 7 and 25% of UK adults reporting feelings of loneliness.
- However, there are large gaps in our knowledge about which groups are more vulnerable to loneliness, the effects this has, and how effective different interventions are.
The 2018 Loneliness strategy was published by the government in response to recommendations by the Jo Cox Loneliness Commission, laying the foundations to tackle loneliness in England. We have expanded on what we know about loneliness since this strategy was launched, thanks to the growing evidence base. However, the COVID-19 pandemic has emphasised the scale of the problem of loneliness and we have set out what we need to know next.
Loneliness has increased during the pandemic, with between 7 and 25% of adults reporting feelings of loneliness. Loneliness leads to multiple and diverse health issues, including a predisposition to mental health disorders, hypertension, and sleeping difficulties. The impact that loneliness has on productivity is becoming clearer, with individuals who are lonely being less likely to do well at school, and more likely to be unemployed throughout their adult life than their non-lonely counterparts. Social isolation associated with the COVID-19 lockdowns is sure to exacerbate the issue of loneliness in the UK. Given the negative effect loneliness has on health and productivity, we need to learn more about how loneliness appears and how to combat it.
Which groups are more affected?
Studies on loneliness have previously looked at specific age groups individually. However, it is now possible to look at how loneliness changes over time. We can also assess how life events can have differing impacts on loneliness for different age groups; for example, how does being widowed at different ages influence loneliness?
We know that loneliness in later life is higher for women with experience of economic hardship and conflictual paternal relationship, and men with experience of prolonged bullying. It is also apparent that certain activities only impact certain age groups of people reporting loneliness – such that the need for social connections at ages 25-34 year affects performance on some social tasks, but does not affect performance of lonely people at other ages.
Effects of loneliness
It is clear that there is an association between loneliness and a range of mental illnesses, with people reporting loneliness being at greater risk of depression. Conversely, there is a link between mental illness and loneliness, with those who are depressed being at greater risk of becoming lonely, highlighting the interconnected nature of loneliness and mental health. Loneliness also appears to be a predictor of suicidal ideation and behaviour across the lifespan, demonstrating the dangerous link between loneliness and mental health.
Factors affecting loneliness
The factors that influence loneliness are varied and complex, and there is a known link between social stigma and loneliness. Experiencing discrimination is one of the strongest predictors of loneliness, which often causes people to shy away from social interactions, while people who are lonely are often perceived as socially inept and poorly adjusted. The impact of sex, sexual orientation, and ethnicity on loneliness have been shown to vary significantly by geographic region highlighting the importance of stigma at the community level.
Living in more remote areas can affect loneliness, due to poor transport and digital connections which can adversely affect social interactions. However, young people also report feeling lonely in densely populated urban areas, while living in greener, more walkable areas reduces loneliness. The factors influencing loneliness are therefore numerous and complex, and solutions must take into account the varying needs of different regions and demographics.
Loneliness is also affected by employment, with studies demonstrating that regions with higher levels of unemployment for 16-24 year olds during the pandemic showing higher loneliness prevalence. In fact, being in work is linked to a lower risk of loneliness, with the nature of the job or work culture also impacting loneliness. As the nature of work rapidly changes, with people changing jobs more frequently and remote working on the rise, it is becoming clear that these different ways of working may impact loneliness. In particular, temporary jobs with short work periods have been found to be associated with loneliness.
The economic case for tackling loneliness
The true cost of loneliness to the UK economy is unclear, although there are estimates of a cost of £2.5 billion a year due to loss in productivity and staff turnover. It is not known what the investment return is for loneliness interventions. Loneliness intervention trials should embed evaluations and economic analysis to ascertain the investment returns to gauge the economic feasibility of such measures. Currently, much of the existing evaluation literature has focused on small scale, short term evaluations, but there is a need for an assessment of longer term economic evaluation – perhaps coordinated between the Department for Work and Pensions, the Department for Digital, Culture, Media and Sport, and the Department for Health and Social Care.
Effectiveness of interventions
A number of studies have investigated the effectiveness of loneliness interventions across several age groups with differing methods of intervention. However, most studies look at older people and in Western countries. A study in 2021 concluded that interventions with the primary aim of reducing loneliness were effective across several age groups. To ensure effectiveness, such interventions will have to be targeted to the correct demographic and several interventions combined to reduce loneliness.
Recommendations
Tackling loneliness will require a targeted approach with the need to prioritise those in groups with pre-existing health conditions and those at increased risk of marginalisation and prejudice, because they are at a higher risk of loneliness and social isolation. Interventions should also be targeted to those known to be at the highest risk of chronic loneliness which we know leads to mental health problems, so interventions should prioritise children in care, care leavers, asylum seekers and refugees, people who are LGBTQ+, people with disabilities, and certain ethnic groups, as well as several other groups. Determining which interventions work best for certain groups will be key to a targeted approach, and the needs of each group will need to be addressed if interventions are to effectively tackle loneliness.
Place-based factors are likely to impact loneliness, but we need to learn more about those risk factors and how they specifically relate to loneliness. How does place impact relationships to loneliness we see in the data, and importantly, what do people need or want from their communities to prevent loneliness?
If we are to tackle loneliness, we need to develop tools that can measure the impact of loneliness on people’s lives. Integrating this into existing quality of life and well-being measures will give a better picture of the true impact of loneliness. High quality evaluations of loneliness interventions are also needed, if effective and robust interventions are to be developed at scale.
Tackling loneliness, along with its impact on mental health and the economy, requires better understanding of how loneliness develops and affects different groups. Crucially, we must also evaluate the cost effectiveness of interventions on loneliness. Combatting loneliness will ultimately lead to a better connected, healthier, and more productive society.


Why do teachers need to think about student experiences of loneliness?
Professor Pamela Qualter, Dr Rebecca Jefferson, and Dr Lily Verity
Globally, many governments have set an objective to reduce loneliness, including among adolescents. So far, however, the focus has been on individuals, and is most often out of school time. In this article, Professor Pamela Qualter, Dr Rebecca Jefferson, and Dr Lily Verity discuss their work in the UK, and internationally, and argue whole school approaches can reduce child and adolescent reports of loneliness.
- The school environment is essential in understanding youth loneliness.
- But most interventions are aimed at individuals, and don’t take into account the larger social system, including the social relationships students have with each other, and with their teachers.
- Research from The University of Manchester has identified different factors in schools and classrooms which can be utilised to reduce loneliness among students.
What is loneliness, and why is it important?
Loneliness occurs when a person thinks their interpersonal relationships are insufficient in some way. It could be that the person is unhappy with the number of social contacts they have, with the closeness and quality of their social relationships, or that their need for social connection is unmet. It is a subjective experience, accompanied by painful or negative emotions. In interviews we have conducted with children and adolescents, they describe loneliness as a painful and sad experience, often accompanied by a perceived lack of belonging or connectedness, particularly to their peers.
Evidence suggests that while loneliness is transitory for most people, for others it can trigger thoughts and behaviours that lead to a prolonged experience. In our interviews with children and adolescents, they talk about prolonged loneliness as having no-one, or feeling like nobody cares about them; and are hopeless that the situation will improve. Such deep pessimism might explain why loneliness is linked to suicide ideation, self-harm, and suicide attempts. There is also substantial evidence that links between loneliness and poor academic and employment outcomes.
Who are the lonely students?
There are a range of risk factors for loneliness among young people that operate across multiple levels of the socioecological model (interrelations among various personal and environmental factors). Generally, the literature focuses on individual risk factors, but the school climate has been shown to be important for understanding loneliness. In our recent work, we have shown that schools’ disciplinary climate, teacher support and interest, peer cooperation, victimisation and discrimination levels are important in understanding student loneliness. Changing school environments so that they are inclusive and more cooperative is key to decreasing the experiences of loneliness among students. Supportive, interested, non-discriminative and accessible teachers are crucial to that change. A school climate encouraging cooperation between students can further mitigate loneliness – the development of guidance and training for teachers by the Department for Education (DfE) is a first step to creating this environment.
Our work suggests that good teacher-student relationships and student-student support can help reduce child and adolescent loneliness. Students’ relationships with their teachers and peers which include the recognition, understanding and acceptance of differences are particularly important. These findings indicate specific aspects of school climate that could be targeted by future interventions to support social connection and reduce the likelihood of loneliness.
Most loneliness interventions for young people are focused on the individual, and so are targeted at children who report loneliness. Those are important, but our work suggests that targeting school factors should also reduce reports of loneliness and prevent some of the experiences from occurring in the first place. Creating supportive teacher-student relationships, encouraging inclusivity, and using an authoritative disciplinary style should lead to increased social connection, and fewer reports of youth loneliness. Integrating these principles into teacher training is one avenue that could be explored by DfE, though policymakers should be mindful of the high workload experienced by the teaching workforce, and ensure guidance on social health is a priority in training. DfE should also consult on the creation of a ‘toolkit’ of techniques and best practice for school staff to draw on, to help embed these principles in the classroom.
School-based interventions for loneliness
Loneliness impacts the health and educational outcomes of young people, but there are few actions taken by schools and teachers to mitigate those effects. That is despite the fact that school and its social environment are associated with student loneliness. We have shown that currently available interventions focusing on loneliness among children and adolescents have been aimed mostly at the individual level, targeting either social and emotional skills (both separately and combined), increased social interaction, enhancing social support, and psychological therapy. These targets are directly linked to drivers of loneliness at the individual level and are reasonably effective. However, such interventions are often expensive, and require intensive training of teachers. They also require important insight from teachers which can make addressing loneliness feel cumbersome. That need not be the case.
Indeed, our research suggests that attending to the psychosocial climate in schools is a manageable way to promote social connection. Making changes to the school environment is effective for decreasing reports of loneliness and is within the reach of most schools and teachers. This is particularly significant given that past research has shown that although teachers acknowledged that schools should seek to enhance students’ well-being, they often feel ill-equipped to do so. We acknowledge that teachers may not necessarily have the specialist knowledge and skills needed for the types of individual-level interventions that target students who report loneliness, and so local authorities have a role in integrating mental health service pathways (where available) into local schools, to ensure teachers have a clear referral route. It is well within the reach of schools and teachers to work, proactively and intentionally, to enhance aspects of the school climate – with the support of DfE, and local education authorities.
Looking forward after COVID
Creating a positive school environment, with teacher- and classmate-support, and an inclusive and protective school community, will have significant benefits for child and adolescent reports of loneliness. Following the COVID-19 pandemic, students need those protective and inclusive environments more than ever.
We have argued elsewhere that such school-based approaches will need to be developed jointly with local students to consider the specificities of each setting, including school facilities and constraints, and the composition of the student and teaching body. This engaged approach is likely to ensure buy-in from the students, which is essential for the success of any intervention.
Tackling loneliness is not just a moral or ethical issue – it is one that is grounded in health and economic realities. In 2017, a report estimated the cost of loneliness to employers at £2.5 billion, and this figure is likely to have increased in the six years since. With adolescent years a key formative period for mental health in adult life, intervening at school-level makes sense for wealth, health, and – most importantly – the quality of life for our children and young people.


All sorted now?
The continued risk of COVID-19 to patients with severe mental illness
Dr Lamiece Hassan and Dr Joseph Firth
The success of the coronavirus vaccine rollout in the UK and internationally has allowed some return to normality for many people. However, one group that was – and continues to be – at risk of being overlooked in the context of COVID-19 is those with severe mental illness (SMI). In this article, Dr Lamiece Hassan and Dr Joseph Firth outline the findings of new research into the continued risk coronavirus poses to those with SMI, and what policymakers and public health officials can do to protect this vulnerable group from the current (and future) pandemics.
- Even after the vaccine rollout, people with SMI remain up to three times more likely to die from COVID-19.
- There is strong overlap between SMI and other risk factors, such as physical illnesses; but these do not account for all the extra risk faced by those with SMI.
- National and local government must develop long-term strategies to understand the issues faced by people with SMI, including tackling mental and physical health inequalities.
People with severe mental illnesses (SMI) – like schizophrenia, bipolar disorder and major depression – have been hit harder by the COVID-19 pandemic. In the first year of the pandemic, previous research (including our own studies), showed that people with SMI were more likely to catch COVID-19 and to suffer serious outcomes as a result. These studies helped to make the case why people with SMI needed extra support and priority access to vaccinations to protect them.
Fast forward a year or so, and vaccinations (and boosters) have become widely available, most social restrictions have been removed, and life is beginning to return to ‘normal’. But when it comes to people with SMI, a key question is; how concerned do we still need to be about protecting people from COVID-19?
Our recent research has aimed to answer this question, examining how people in Greater Manchester with SMI were affected by COVID-19 before, during and after vaccinations become available.
We looked at anonymised patient records from almost 1 million people with different mental illnesses, including their medical history, vaccinations and COVID-related outcomes like infections, hospitalisations and deaths. Our sample included people living with schizophrenia, bipolar disorder, and major depression, compared against records of patients with no history of mental illness. The sample was followed up from February 2020 until September 2021.
We found that after the vaccine roll-out began in December 2020, death rates due to COVID-19 declined across all groups of people, regardless of diagnosis. However, people with SMI were still more likely to die from COVID-19 compared to their matched counterparts without prior mental illness. Overall, this risk of death was about three times higher for people with schizophrenia and bipolar disorder, and 1.5 times higher for people with a history of major depression.
Underlying physical illnesses (like diabetes, cancer and heart disease) were more common among people with SMI than their matched counterparts. We also saw that vaccination rates by September 2021 varied among people with SMI: the rate of double vaccination was highest among people with major depression (74%) and lowest among people with schizophrenia (66%). When we took into account the impact of underlying physical illnesses and vaccination, this accounted for some, but not all, of the extra risk we saw among people with SMI. This means it is likely that other factors may be at play among people with SMI that we didn’t consider, or haven’t yet been identified.
This research – one of the largest studies of its kind in the world – was only possible because we had access to a large dataset of anonymised records from people in Greater Manchester, known as the GM Care Record. Wider moves to digitise and integrate patient records on a national scale, and to build secure analytics platforms suitable for research use, should make studies like this even easier in future.
Even so, it is challenging to conduct this kind of research. For one thing, we based our groupings of people on lifetime diagnoses (if they had ever/never had a specific diagnosis), which doesn’t take into account the severity or recency of illness. Furthermore, people may have had more than one diagnosis of SMI in their lifetime, masking some of the differences between groups. To unpick some of these complex issues, we worked with experts in statistics and people with lived experience of mental illness (and their carers) to help us interpret the results carefully.
What does this mean – and what can we do about it?
In summary, our research shows that people with SMI, and particularly those with schizophrenia and bipolar disorder, are still more likely to be at risk of dying from COVID-19, even after the vaccination roll out. Thankfully, deaths may be lower overall now, but the differences in relative risk are still arguably cause for concern. Strategies for preventing serious illness and death from future pandemics – including new COVID variants – should understand this risk and seek to mitigate it. This requires clear communication to and from public health bodies that those with SMI are a vulnerable group, alongside specific interventions to protect this group from infection.
We should be mindful that people with SMI also showed an increased risk of death due to causes other than COVID-19 through the study: so these risks of COVID-19 can be interpreted as added risks on top of those health inequalities that people usually face. Policymakers in national and local government, and in health and social care services, should take steps to understand the causes of these health inequalities, and how they might be mitigated to ensure this group is not at greater risk of serious illness and death. Policymakers must also be mindful of how poor mental health intersects with other factors associated with health disparities, such as lower income, age, and ethnicity.
Clearly, we need to understand reasons why people may or may not be vaccinated, and offer support and information. Indeed, we saw significant numbers of individuals who remained unvaccinated, which is concerning. Healthcare professionals should actively offer, discuss, and record attempts to promote vaccination in this group, where they are eligible. Efforts should be made to understand the reasons for vaccine hesitancy, particularly among people living with schizophrenia.
Finally, given the higher risks of physical health problems that people with severe mental illness suffer from, we need to resume regular physical health checks that may have taken less priority during the pandemic. Over the longer term, the impact of research like ours adds pressure on policymakers to address physical, as well as mental, health problems among people with severe mental illness to increase the quality and years of life.

Mind your language
Interpreters in Mental Health Act assessments
Professor Alys Young, Dr Rebecca Tipton, and Dr Natalia Rodríguez-Vicente
In England and Wales, the Mental Health Act can be used to detain people experiencing a mental health crisis, and who may pose a danger to themselves or others. However, some of those assessed under these powers will not use spoken English. Here, Professor Alys Young, Dr Rebecca Tipton, and Dr Natalia Rodríguez-Vicente explore the effects on the assessment process, equity, and outcome when an interpreter is involved, and how policymakers can ensure better regulation and data collection.
- In 2020-21, there were over 53,000 detentions under the Mental Health Act 1983.
- It is compulsory to collect data on ethnicity and gender – but not the language of the person being assessed.
- There are no minimum or regulated training requirements for interpreters taking part in statutory Mental Health Act assessments, as well as a lack of understanding from assessors on how to work with interpreters in the process.
- Without additional requirements to audit language characteristics and interpreter use (alongside ethnicity and gender), potential inequities in practice and outcome of assessments cannot be identified.
- Evidence-based co-training of interpreters and mental health professionals would transform practice.
Few pieces of legislation can result in the deprivation of a person’s liberty on grounds of health. One of these is the Mental Health Act 1983 (MHA), which is law in England and Wales and is similar to legislation in other countries of the UK and around the world. The MHA allows for the formal assessment of a person experiencing serious mental ill-health and who might be a danger to themselves or others, and can result in their compulsory detention in a suitable psychiatric facility for assessment, treatment, protection, and care.
In addition to psychiatric assessment, Approved Mental Health Professionals (AMHPs) apply a social care perspective at the point of assessment to ensure that options other than compulsory admission are investigated, the perspective of the person being assessed is taken into consideration, and their best interests are safeguarded. In 2020-21 there were over 53,000 detentions under the MHA. But what happens if your first, preferred, or only fluent language is different from spoken English, and you undergo assessment under the Mental Health Act?
Ethnicity and language
Proposed legislative reforms to the MHA are addressing disparities in assessment and outcome. In 2020-2021 rates of detention for the ‘Black or Black British’ group (341.7 detentions per 100,000 population) were over four times those of the ‘White’ group (72.4 per 100,000 population). However, attention to diversity in ethnic identity is not synonymous with a focus on diversity in language use.
Although gender and ethnicity are part of the minimum data set annually reported for MHA monitoring purposes, language is not. There are no national data sets on the preferred/first language of those assessed under the MHA, nor how many undergo an assessment where a spoken and/or signed language is required. This lack of attention is particularly surprising given the needs of migrants, refugees, and asylum seekers within the mental health system, and the increasing linguistic diversity of the UK. Census data for England and Wales records that 4.1 million people (7.1%) of the overall population were proficient in English but did not speak it as their main language. Furthermore, of the 5.1 million (8.9%) who did not report English as a main language, 17.1% (880,000) could not speak English well and 3.1% (161,000) could not speak English at all.
The INForMHAA (INterpreters For Mental Health Act Assessments) research project, led by The University of Manchester, has been investigating:
- Dilemmas faced in joint working between interpreters and AMHPs.
- What is most valued from the perspective of a person being assessed if an interpreter is involved.
- How to improve interpreter-mediated assessments in practice.
Interpreting in MHA assessments
Responsibility for effective communication in an MHA Assessment is shared, with AMHPs holding statutory powers and interpreters handling the inter-linguistic and inter-cultural exchanges. This distribution of responsibility means that there is a high need for and reliance on effective interprofessional working that combines both skillsets. Most interpreters will have little prior knowledge of working in mental health, let alone within an MHA assessment. Few AMHPs will have additional specialist training in working alongside interpreters. ‘Learning on the job’ is a common experience for both sets of professionals but this is occurring in a high stakes situation where compulsory detention may be the outcome for the person assessed. The appropriateness of this is questionable.
AMHPs have significant statutory responsibilities including ensuring great efforts are made to inform an assessed person of their rights, options, and consequences of what is happening. They have to assure themselves that what they need to say has been fully conveyed to the person being assessed; this is hard to know if you do not share their language. It can lead to them asking interpreters to ‘just translate what I say’. However, terminology such as ‘capacity’, ‘section’, ‘objection’, ‘voluntary admission’ have specific meanings and implications in the context of the MHA. An interpreter may understand the word, but their choice of vocabulary or expression to match it may not be nuanced enough for this particular circumstance. Word knowledge and language usage are not the same thing.
People may express themselves in a disordered manner when experiencing a mental health crisis. How they are using language is a vital window for AMHPs to understand the ways in which their mental health is being affected as well as their wishes. Sometimes people use inappropriate vocabulary, speak or sign at a faster rate, talk or sign but just don’t make sense. Interpreters without specialist training may see their job as making sense of what someone is saying, tidying up the language, or ensuring communication is smooth. In this context, that is misleading.
Professional regulation
AMHPs are highly trained, registered professionals whose standards, conduct and work are formally monitored to maintain registration. Conversely, there is no compulsory, only voluntary registration for spoken language interpreters in the UK. There is no minimum standard of qualification to work as an interpreter (although there is a recommended one), resulting in people who may be bilingual but who have never trained as an interpreter working in statutory contexts. There is a voluntary code of conduct and ethics, but without formal registration no consistent process of listing an interpreter as unsuitable or sanctioned. Sign language interpreting is in a different position, with postgraduate level qualification in interpreting leading to registration – but not statutory regulation.
Implications for policy
Without routinely collected data on use of interpreters and preferred languages of those assessed under the MHA, potential inequities in outcomes and standards of practice cannot be adequately monitored. Evidence-based guidance on working alongside interpreters in MHA assessments should be implemented to improve practice and reduce inequities.
The lack of qualification standards leading to formal registration in public service interpreting creates significant vulnerabilities in accountability in enacting a statutory duty and responsibility. A minimum standard of qualification with additional specialist training for working in statutory practice should be introduced for interpreters.
Extension training for AMHPs to work alongside interpreters and interpreters for working specifically in statutory mental health circumstances is required for standards of practice to improve.
In drafting new legislation and statutory guidance, the importance of disparities in process and outcome arising from language should be addressed to the same extent as those arising from ethnicity or gender.
Evidence-based professional guidance and training resources aimed at AMHPs and spoken and signed language interpreters will be available in early 2024 via the project website.
This project was funded by the National Institute for Health and Care Research School for Social Care Research (grant number P172). The views and opinions expressed therein are those of the authors and do not necessarily reflect those of the NIHR SSCR or the Department of Health and Social Care.
The full research team also includes Jemina Napier, Chair of Intercultural Communication, Heriot-Watt University; Sarah Vicary, Professor of Social Work and Mental Health, Open University; Celia Hulme, NIHR Post-doctoral Fellow, The University of Manchester.


Locked up like adults
COVID-19 experiences for children in custodial settings
Dr Charlotte Lennox
During the early period of the pandemic, there was a lack of detailed guidance for many groups, including the secure estate. For children in custodial settings, this meant staff often applied measures intended for adult prisons, in lieu of any other information. Here, Dr Charlotte Lennox shares her research showing children in such settings were an invisible group during COVID-19.
- During the pandemic, no single government department had responsibility for implementation of COVID-19 guidance for children in custodial settings.
- Children were confined for up to 23.5 hours a day, with a significant impact on their mental health and wellbeing.
- Clear lines of accountability, better future planning, and a review of current measures are needed to avoid this happening again.
Children in custodial settings have much higher rates of mental health and neurodevelopmental disorders than children in the general population. Prior to the COVID-19 pandemic, HM Inspectorate of Prisons (HMIP) repeatedly expressed concerns about the safety of children in custodial settings. Now, evidence suggests that COVID-19 restrictions and limited social interactions had a significant impact on the general population, and a disproportionate impact on young peoples’ mental health. As children in custodial settings were an already vulnerable group, there were concerns about the impact of the COVID-19 restrictions.
Researchers led by Dr Lennox undertook a study aimed at understanding this impact, combining HMIP and Ofsted reports with analysis of policies, and the effect of these policies on children, staff, and settings. They also interviewed 41 participants, including NHS staff, policymakers, and children with experience of custody during COVID-19.
Findings
This research found that there were direct and indirect impacts of the COVID-19 pandemic, and the policies implemented.
Direct impacts
Children were not considered when COVID-19 guidance was being developed for custodial settings. There was no consistency of approach across the three site types - Secure Children’s Homes (SCH), Secure Training Centres (STC) and Young Offender Institutions (YOI) - and no single government department had oversight. This resulted in most sites adopting, to differing degrees, the COVID-19 guidelines for the adult prison estate.
However, this meant that children were locked in their rooms, in the worst cases for 23.5 hours a day for weeks at a time. The smaller SCH sites were able to offer more time out of their room, but during lockdowns, on admission, and periods where children needed to self- isolate, they did this time on their own, locked in their rooms. This isolation did result in a deterioration of children’s mental health, and within the NHS England Children and Young People Indicators of Performance (CYPIP) data, we saw increased referrals once restrictions were lifted with referrals higher than pre-COVID-19 rates.
‘Bubbles’ were one of the main ways sites managed children. Initially these were successful, as the smaller groups made it easier for staff to manage behaviour, keep good communication, and develop staff and child relationships. However, over time these bubbles led to rising tensions and inter-bubble conflict, as children within them formed gang-like relationships. These issues were more apparent in the larger sites than within the SCHs.
Data from our interviews showed that the rollout of the COVID-19 vaccination programme, and conflicting messaging and behaviours from residential staff around vaccine take-up, appeared to have an impact on childhood vaccinations more generally, with an increase in refusals for all vaccinations.
Indirect impacts
COVID-19 and policies implemented to minimise transmission affected staffing levels. These low staffing levels subsequently impacted many aspects of life, including how the children’s behaviour was managed, their ability to access facilities, services and professionals, and ultimately further restrictions and isolation. Staffing issues were more acute in the larger sites.
Prior to COVID-19, NHS England commissioned ‘The Framework for Integrated Care’, (SECURE STAIRS) to improve the quality of care for children. It aimed to do this through culture change, promoting trauma-informed, formulation-driven, and delivered within a whole-systems approach. In March 2020, sites were at varying stages of implementation. While the CYPIP showed that the number of children with a formulation had actually increased over time, our interview data suggested that in some sites staff had struggled to maintain momentum. The Framework for Integrated Care (SECURE STAIRS) needs significant staff training and reflective practice, and these were the first things to be cut due to staffing shortages.
Policy recommendations
Future pandemic planning:
The lack of oversight of custodial settings by any single government department was central to the problem. To avoid repetition of these mistakes, a more coordinated strategy is needed between the Ministry of Justice, the Department for Health and Social Care, and the NHS. This includes having direct lines of accountability and advocacy for children in custodial settings when developing any policy.
There is a need for consistent infection control policies that are suitable for children in all custodial settings. In the future, if isolation periods are needed, this should be for the shortest amount of time, the needs of the child should be paramount, and there should be effective senior leadership in monitoring of isolation. There is a need to support the larger settings to encourage childhood vaccinations uptake given the increase in refusals.
Lessons learned from COVID-19:
The use of bubbles over time within the larger sites has been problematic. While the direction of travel is for smaller Secure Schools, this study highlights some important considerations, particularly around group dynamics. In the larger sites, there is also a need to address staffing issues in order to improve staff-child relationships and behaviour management.
Areas of practice to be refreshed:
The introduction of the Framework for Integrated Care (SECURE STAIRS) is likely to deliver improvements in children’s care. However, it requires sustained buy-in from all sectors, we would urge a drive to refresh uptake by the custodial settings. The use of the CYPIP data has the potential to be an effective research tool, but sites need to understand the value of reporting on this data to improve data quality.
Summary
While younger age groups so far seem to have endured a smaller physical toll from the pandemic, the same cannot be said for emotional and mental trauma – with children in the secure estate particularly affected. As with children more generally, it was assumed this group would help spread the virus, though this appears not to be the case.
This research demonstrates the necessity for clear and separate strategies for children living in the secure estate (particularly larger sites), alongside a single route of decision-making responsibility – and accountability.
The outcomes of the pandemic are still being explored and being used to strategically plan for future outbreak management. Children and young people must be a central part of this, including those on the secure estate.
This project is not supported by HM Prison & Probation Service or Youth Custody Services. The views expressed are those of the author and not necessarily those of the National Institute for Health and Care Research or the Department of Health and Social Care.


Mind the gap
Supporting prison leavers with mental illness
Dr Jane Senior, Professor Jennifer Shaw, and Dr Charlotte Lennox
Many people in prison have severe mental health problems, but what is being done to help these individuals resettle when released? And how can policy and practice reduce reoffending rates, while ensuring prison leavers with mental illnesses are given the support they need to reintegrate into the community? Here, Dr Jane Senior, Professor Jennifer Shaw, and Dr Charlotte Lennox outline their research into Critical Time Interventions, and what the evidence says about how best to help prisoners get back into society.
- Without bespoke and ongoing support, many prisoners with mental health needs lose contact with community services when released.
- Critical Time Intervention is one model for helping these prison leavers reintegrate into communities, and has been shown to lead to better outcomes.
- A more joined-up approach to prison resettlement is needed for leavers with mental health needs, which could help lower rates of reoffending, and ease pressure on the NHS and community health services.
Since the 1999 Future Organisation of Prison Healthcare report, attempts at healthcare for prisoners has been delivered as a partnership between the NHS and the Prison Service. And since 2013, responsibility for commissioning all healthcare services for prisoners in England – with the exception of emergency and out-of-hours services – has rested with NHS England. Within the community, Integrated Care Boards (ICBs) are responsible for commissioning the majority of healthcare services for prison leavers, having inherited this responsibility from the now defunct Clinical Commissioning Groups.
But how is the handover between prison and community services managed?
Earlier research led by The University of Manchester found that, of 53 prisoners who had been in touch with in-reach services, and who had severe and enduring mental health conditions, just 4 were in contact with community mental health services six months after release. The study concluded that there “is a need for robust discharge planning and proactive through care for prisoners with mental health problems”.
What else can be done – and what works?
Critical Time Intervention
Critical Time Intervention (CTI) is an American model of care, designed for people in psychiatric hospitals who were discharged as homeless. It involves the development of holistic discharge packages, to organise all the services and needs that patients have said are a priority to them. This includes funding, accommodation, education, and employment alongside healthcare needs. CTI managers (who are clinicians, routinely nurses) work with patients both before and for a short period following their discharge, to ensure they have stable pathways and support in place.
A review of CTI in the US found that patients who received support from this model were less likely to be homeless, and spent less time using emergency care facilities, than the ‘treatment as usual’ (TAU) group.
Researchers from The University of Manchester wanted to know if this model could be applied to prisons. They adapted the training manual for CTI managers, to cater to the needs of prison leavers. They were as follows:
- Ensuring prisoners on remand were able to attend court dates with arrangements in place (such as medication supplies, appointment with community services) should they be released.
- Registering prison leavers with GP services in the areas they were discharged to.
- Liaising with statutory and third sector organisations, plus families and other community links, around providing accommodation, where this was possible.
Findings
It was found that people who went through CTI were significantly more likely to remain in contact with mental health services, and to be concordant with their medication, than those who didn’t. This was true at 6 and 12 months after release. However, a loss of contact following 12 months will lead to CMHT and NHS incurring significant further costs and pressures, and demonstrates that CTI alone is no magic bullet. Prisoners with severe mental health issues require the same kind of life-long support that would be provided to any patient with these conditions, and this must be recognised in a joined-up strategy between the Ministry of Justice, and the Department for Health and Social Care.
Researchers also found that, in addition to better outcomes, CTI was liked by both prison leavers and staff, with a common notion that it was the ‘right thing to do’, and that working in this intensive way provided ‘proper’ mental health care. CTI participants were less anxious about release, and reported receiving more support with housing, access to services, and community reintegration, than during previous periods of incarceration, due to being closely supported by their CTI manager.
However, it is reasonable to expect that, when moved to the status of receiving routine Community Mental Health Team (CMHT) support, with less frequent contact and intensive CTI management, contact and engagement will wane, potentially leading to continued mental illness and criminality. As such, the move from prison to the community should include wider CTI training for CMHT services. CMHT staff will need CTI training, and the time and resources to dedicate to their clients. This could be done by having CMHT staff who have reduced caseloads of only CTI clients, or giving all CMHT staff a small number of CTI clients along with a reduced ‘normal’ caseload.
Recommendations
CTI has not been widely adopted to date, in part due to higher costs than the standard model of release. However, given that it showed significantly better outcomes for prison leavers with severe mental health issues, it is likely that its use could lead to net savings overall, through wider economic benefits to public services through lower use of emergency care, better community integration, and reduced rates of reoffending.
- The Ministry of Justice should commission research to investigate the wider health economics of CTI.
CTI is no universal solution – a related model (‘Engager’), when trialled found that, for prisoners with more mild mental health conditions, the results were mixed. However, for those prisoners with the greater mental healthcare need, the evidence shows that CTI has the potential to be a powerful asset in the wider toolkit for improving community resettlement, and helping prison leavers to lead fulfilling lives outside the justice system.



Contributors
Joseph Firth
Dr Joseph Firth is a UKRI Future Leaders Fellow in the Division of Psychology and Mental Health at The University of Manchester. Joe’s current research primarily focuses on the use of digital technologies and physical health interventions for improving both physical and mental health.
Lamiece Hassan
Lamiece Hassan is a Research Fellow in the Division of Psychology and Mental Health at The University of Manchester. Recently her research has primarily investigated links between mental illness and COVID-19 outcomes. Lamiece’s main interests are in using digital health and real-world data sources to generate insights about mental and physical health.
Neil Humphrey
Professor Neil Humphrey is the Sarah Fielden Chair in Psychology of Education at The University of Manchester. His research focuses on what we mean by mental health, why mental health matters, what matters for mental health and what works for mental health in children and young people.
Rebecca Jefferson
Rebecca Jefferson is a Post-doctoral Researcher at The University of Manchester and Lecturer in Clinical Psychology at the University of Central Lancashire. Her research explores adolescent loneliness in the context of school climate as well as gendered contributors to psychological distress in adolescent girls. Her research also explores the impact of obesity on quality of life.
Charlotte Lennox
Dr Charlotte Lennox is a Chartered Psychologist and criminal justice health researcher at The University of Manchester. Her research focuses on improving health outcomes for people in contact with the Criminal Justice System by influencing policy, practice, and service delivery. She has a specific interest in young people in contact with the Criminal Justice System.
Jo Neill
Jo Neill is Professor of Psychopharmacology at The University of Manchester. She is Chair of the Medical Psychedelics Working Group at Drug Science, a Trustee for Heroic Hearts UK, and a scientific advisor for the Conservative Drug Policy Reform Group, Beckley Psytech, Albert Labs, and Octarine Bio. Jo is also an advisory board member of the International Therapeutic Psilocybin Rescheduling Initiative, and co-founder of b-neuro, a University-based Contract Research Organisation developing new treatments for mental illness through animal models.
Pamela Qualter
Pamela Qualter is Professor of Psychology for Education at The University of Manchester. Her research explores child and adolescent peer relationships, including their experiences of loneliness and its impact on mental and physical health and social functioning.
Natalia Rodríguez-Vicente
Natalia is a lecturer at the University of Essex where she teaches courses on conference and public service interpreting. Her research focuses on the intersection between language, culture and mental healthcare provision with a focus on interactional pragmatics. Her PhD thesis on language mediation in Psychological Medicine was granted international recognition by winning the 2021 CIUTI award.
Cathryn Rodway
Cathryn has worked in mental health and suicide prevention research at the Centre for Suicide Prevention for over fifteen years. She is currently working as Programme Manager at the National Confidential Inquiry into Suicide and Safety in Mental Health (NCISH). Cathryn was co-Investigator for a recent UK-wide study examining suicide by former personnel of the UK Armed Forces and has also led research projects investigating suicide by children and young people and suicide by middle-aged men. Her research interests include suicide in young people, homicide, serious violence and mental health.
Jane Senior
Jane is a Senior Lecturer in Forensic Mental Health and manager of the Offender Health Research Network, The University of Manchester.
Jennifer Shaw
Jenny Shaw has over 30 years’ experience in the NHS, predominantly in Mental Health, currently as a Consultant Forensic Psychiatrist. She has extensive experience of NHS Management, service reviews and service development. She is Professor of Forensic Psychiatry, Consultant Forensic Psychiatrist and academic lead for the Offender Health Research Network at The University of Manchester.
Frances Smith
Frances Smith completed research exploring the use of psychedelics amongst veterans with trauma symptoms while doing her Master's degree in Forensic Psychology and Mental Health at The University of Manchester. She currently works with women who are homeless and are sex working.
Rebecca Tipton
Rebecca is a Lecturer in Interpreting and Translation Studies at The University of Manchester. Her research focuses on contemporary and historical experiences of spoken language interpreting in a range of statutory and non-statutory service settings in the United Kingdom. She has been involved in studies exploring interpreting in adult social work, police interviews and charity services for domestic abuse survivors, aimed at improving interprofessional working practices.
Lily Verity
Lily Verity is a post-doctoral Research Associate working on co-developing a developmentally sensitive measurement scale for youth loneliness. Her research primarily focuses on understanding young people’s experiences of loneliness from their own perspectives through qualitative research approaches.
Verity Wainwright
Dr Verity Wainwright is a Chartered Psychologist and Lecturer in Forensic Psychology and Mental Health at The University of Manchester. Her research focuses on improving health and patient safety in criminal justice settings, including national studies of prison suicide and suicide risk in the criminal justice system, the mental health of ex-armed forces personnel in prison, and risk assessment in medium secure services.
Jodie Westhead
Jodie Westhead is a Research Associate at the National Confidential Inquiry into Suicide and Safety in Mental Health and the NIHR Greater Manchester Patient Safety Research Collaboration. She completed her PhD examining the outcomes of patients admitted to Medium Secure Psychiatric Care in 2020, and since then has led on evaluations of new care models for healthcare services before becoming research lead for the Suicide in Armed Forces Veterans Study.
Alys Young
Alys is Professor of Social Work at The University of Manchester and a NIHR Senior Investigator. Her research focusses on inequalities in health and social care with specific reference to those experienced by Deaf users of British Sign Language and the Deaf community. She has led studies aimed at improving mental health services for Deaf adults and early childhood intervention and support for families with deaf children in the UK and in South Africa.

All opinions and recommendations made by article authors are made on the basis of their research evidence and experience in their fields. Evidence and further discussion can be obtained by correspondence with the authors; please contact policy@manchester.ac.uk in the first instance.
Read more and join the debate at: blog.policy.manchester.ac.uk
@UoMPolicy #OpenMinds
October 2023
The University of Manchester
Oxford Road,
Manchester
M13 9PL
United Kingdom
The opinions and views expressed in this publication are those of the respective authors and do not necessarily reflect the views of The University of Manchester.